Latest developments in anthroposophic-based care for the closing years of life
New workshops for supporting the development of a culture of care, focused on anthroposophic nursing and palliative care, have been announced since this post was published on June 11.
Irmhild Kleinhenz and have several workshops on Anthroposophical nursing techniques, part of their Holistic Home Care series, in the Coffs Harbour area, Lisa Harris and the Palliative Care Initiative are still hoping to run a comprehensive 2-day workshop later in the year; and Rev. Lisa Devine is still hoping to commence her palliative care volunteer training, ‘The Threshold Course’ this October, as the Sydney lockdown ends. The recordings will be available to remote local teams of anthroposophic medical and nursing practitioners.
27 November: Holistic Home Care workshop – Care after Death Demonstration. Please contact Irmhild Kleinhenz or
11 December: Holistic Home Care workshop – Foot Oiling. Please contact Irmhild Kleinhenz or
During our Hearts Online webinar in early June on Diversity, Inclusions and Reconciliation, there were several calls for us to more actively connect and build a culture of care into our community. It’s a theme that stretches across all ages and cultures, but particularly at this time of community social distancing, as COVID precautionary measures become embedded in society as social norms. This hands-off approach has particularly affected older adults, particularly those who are frail, very old, or have multiple chronic conditions. And it only reinforces the sense of loneliness and isolation many feel, as well-meaning families keep their distance and medical practitioners put physical barriers between them and their patients to keep them ‘safe’.
For many elderly people, health is influenced more by their daily lives and social contact than by medical intervention. Facing the challenges of social isolation, they are particularly vulnerable to rapid mental and emotional decline. Care is how we show each other compassion and love, but lack of care has sadly become a hallmark of growing old in Australia. And then there are ever-renewed calls to make voluntary assisted dying legal and available in all states, to ease the suffering of people at the end of their tether – physically, mentally and emotionally – from pain and loss of sense of self. For many doctors and carers, there is a sincere desire to end the suffering of their loved ones this way, but Rudolf Steiner tells us that, in fact, every extra hour we live on earth is important for the whole of humanity. How can we reconcile these two approaches?
The art of ageing
 Growing old requires courage and trust. We all would like to age gracefully and die with dignity, but we don’t always think about how to make this happen. Perhaps we assume our loved ones understand us well enough to provide for us as we would like. Perhaps we think we’ll just worry about it when the time comes. But perhaps we don’t realise how much thought and planning is required to make our final years nourishing and dignified. To this end, many people – nurses, therapists, doctors and priests – in our community believe we need to develop a more conscious and active culture of care for the elderly and the dying.
Growing old requires courage and trust. We all would like to age gracefully and die with dignity, but we don’t always think about how to make this happen. Perhaps we assume our loved ones understand us well enough to provide for us as we would like. Perhaps we think we’ll just worry about it when the time comes. But perhaps we don’t realise how much thought and planning is required to make our final years nourishing and dignified. To this end, many people – nurses, therapists, doctors and priests – in our community believe we need to develop a more conscious and active culture of care for the elderly and the dying.
Although there has been an impulse here in Australia for many years towards providing anthroposophic-based care for older people – Christophorus House is one such venture – there has been a renewed commitment in the last twelve months to a vision of establishing anthroposophic-based services and centres for those who need extra support and love towards the end of life. but there is also the recognition, says naturopath Irmhild Kleinhanz, that we desperately need a new culture of care to realise this, one that looks equally to the physical, spiritual and social needs of our elders, one that puts caring, comfort and community at the centre of the hands-on care model.
Below are just a few of the initiatives in aged care and palliative care that are gathering momentum here in Australia.
Recent webinars
 Last year, Hearts Online ran two webinars to bring this work to a wider audience. A Conversation About Ageing focused on the spiritual dimensions of illness and health during the ageing and dying process. Following on was Planning for the future of Anthroposophic-based aged care in Australia which looked at potential future projects for creating residential aged care services and a palliative care model that aims to spiritualise palliative care beyond simply easing the body towards death as its ultimate goal.
Last year, Hearts Online ran two webinars to bring this work to a wider audience. A Conversation About Ageing focused on the spiritual dimensions of illness and health during the ageing and dying process. Following on was Planning for the future of Anthroposophic-based aged care in Australia which looked at potential future projects for creating residential aged care services and a palliative care model that aims to spiritualise palliative care beyond simply easing the body towards death as its ultimate goal.
Developing an anthroposophic-based aged care facility
Irmhild Kleinhenz, anthroposophic naturopath and a mentor for Anthroposophic Medicine in Australia of many years experience, believes the art of ageing urgently requires a new culture of care that encompasses social co-existence and intergenerational encounters with special nursing care. With Charlotte Rogers (anthroposophic nurse, art therapist and rhythmic massage practitioner), she is pursuing the possibility of developing an aged care facility on the mid-NSW coastal regions of Coffs Harbour and Bellingen. Together they have started a series of monthly home care sessions teaching anthroposophic home-care treatments to carers and other interested parties.
Contact Irmhild Kleinhenz for more information on their work.
The Palliative Care Initiative

Vigil room, Sterriwijer Hospital, Belgium
Dr Lisa Harris is a GP Proceduralist in Palliative Care and an Anthroposophical doctor. At the Hearts Online webinar on planning for aged care, she spoke of her vision for the future of a model of care that will support the spiritual and soul needs of each individual as they approach death. Last year, twenty Anthroposophical medical and allied health practitioners began meeting monthly online to work together to distinguish what Anthroposophy can bring to palliative care in Australia. This year the group, facilitated by Lisa, has commenced a visioning process to define their identity and what services they aim to offer.
The short-term goal is to produce Anthroposophical palliative care education and support local care teams to support dying patients and their families in the community and, if needed, in the hospital. The long term goals are a hospice facility, perhaps a four-bedroom home initially, serviced by Anthroposophical practitioners – nurses, counsellors, GPs, art and massage therapists, naturopaths, supported by biographical work, pastoral care and post-death care.
If you are training in or a qualified Anthroposophical practitioner or priest interested in joining this circle, please contact Lisa Harris
Palliative care nursing
Pippa White is a freelance palliative nurse with additional training in anthroposophical nursing care. Based near Melbourne, Victoria, she teaches home-based treatments for parents of young children and offers anthroposophical nursing treatments, as well as end-of-life nursing support. She regularly offers workshops with Rev. Cheryl Nekvapil (Melbourne) or Irmheld Kleinhanz (Coffs Harbour) on how to approach death and dying with a spiritual perspective.
You can listen to Pippa talk about her work here.
Educating people about ageing and palliative care.
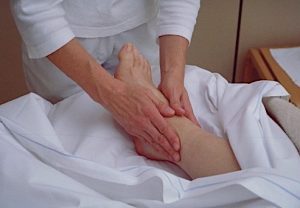 Educating people about the art of ageing and the need for a new culture of care is a major impulse this year, with a focus on nurse education, home and post-death care workshops and training in how medical practitioners work with priests at this sacred threshold of death.
Educating people about the art of ageing and the need for a new culture of care is a major impulse this year, with a focus on nurse education, home and post-death care workshops and training in how medical practitioners work with priests at this sacred threshold of death.
If you are interested in reading more about the need for a comprehensive and spiritual approach to palliative care and the anthroposophic stance on assisted dying, here you can read this statement from the Goetheanum’s Medical Section on the subject.
Join our survey and emailing list!
We are running a survey on members’ interests in ongoing workshops on a range of topics associated with ageing, death and dying. So far there has been substantial interest in workshops on nursing practices and pastoral care, but also for creative activities to support healthy ageing and biographical work at the end of life. You can do the survey here.
We will then add your contact details to our email list to let you know directly about major upcoming events on the art of ageing, aged care support, palliative care, and end-of-life.
But also keep your eyes open for workshops and seminars on these themes in your area or contact your local branch coordinator.
And if you are an anthroposophic medical/therapeutic practitioner with an initiative in aged care or palliative care that you would like to share, please contact me.
Fiona Campbell
Spiritually speaking, one aspect of growing old is that we squeeze out something spiritual here on earth. We are, however, very close to the point today where people fall into the worst errors concerning the above. Even truly well-meaning people are liable to fall into error with regard to the above. The errors will grow and grow and may even assume gigantic proportions as earth evolution continues.
Rudolf Steiner PhD: an extract from his lecture on Cosmic Intelligence and Speech
GA183 Lecture 2nd of September 1918. Reprinted in the Circular Letter No 12 1995.